Prolistem® Treatment Stages
PHASE ONE
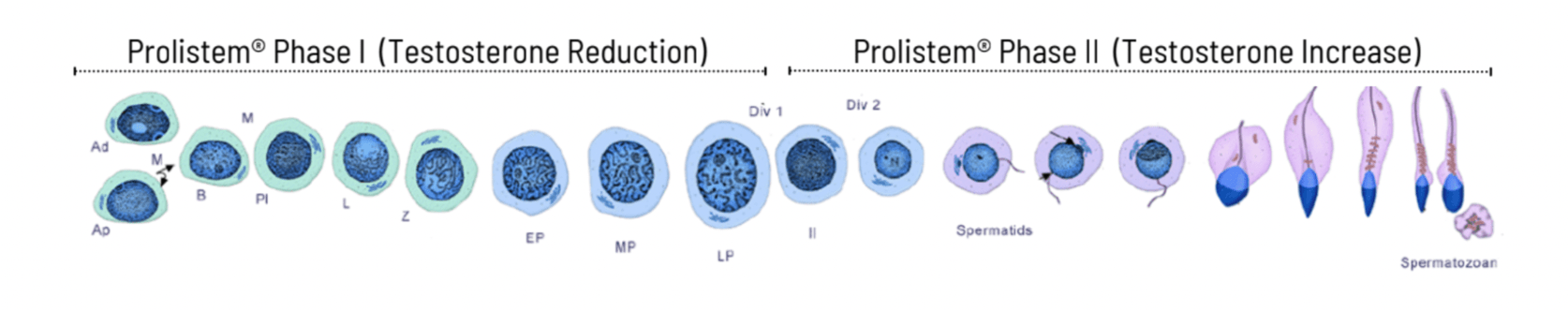
Stage One and Two
Prolistem® is a comprehensive and targeted solution for men struggling with non-obstructive azoospermia. Through a two phase treatment process, Prolistem® increases the chances of reproductive success for men with this condition.
Phase one of the Prolistem® treatment (three bottles over three months) focuses on increasing the number of spermatogonial stem cells which are responsible for testicular stem cell function, and promoting differentiation into the next stages of sperm production by naturally lowering testosterone levels and increasing growth factors that promote their growth.
Prolistem® phase one uses the active component of licorice, glycyrrhizic acid, which is hydrolyzed in-vivo to glycyrrhetinic acid, to block 17β-hydroxysteroid dehydrogenase (17βHSD), which catalyzes the conversion of androstenedione to testosterone. In addition, Prolistem® uses flaxseed, which is rich in Omega-3 fatty acids that may be linked to a decrease in testosterone levels. in addition small amount of Maca roots and Tribulus Fruit
Stages one and two contain supportive vitamins: Vitamin A, Thiamin, Folate, Vitamin B12, and Iodine
PHASE TWO

Stage Three
Phase two (Stage Three Bottles) of the Prolistem® treatment is designed to enhance sperm count, motility, and quality. During this phase, testosterone levels are restored to normal to facilitate healthy sperm production.
Stage three of our product consists of clinically approved ingredients specifically chosen to support sperm health.
Vitamin A, Vitamin C, Vitamin D, Vitamin E, Thiamin, Riboflavin, Niacin, Vitamin B6, Folate, Vitamin B12, Pantothenic Acid, Calcium, Iodine, Magnesium, Zinc, Copper, Grape Seed Extract, Epimedium, Pomegranate, Velvet Bean Seed, Damiana Leaf, Ginkgo Leaf, Asian ginseng Root, Maca Root, Tribulus Fruit, L-Arginine

